On Tuesday, the Los Angeles County Board of Supervisors voted to launch a two-year pilot program that seeks to add 500 mental health care beds across the county.
“For far too long, the number of mental health beds in this county and across the state have dwindled,” the motion’s author, Supervisor Kathryn Barger, said on Tuesday. The dearth of beds means that mental health patients often cycle in and out of county jails and on and off LA’s streets.
Top mental health experts estimate that the minimum number of mental health beds required to adequately serve the public’s needs is 50 beds per 100,000 residents. As of the beginning of this year, Los Angeles County only had about 22.7 beds for every 100,000 people. And in all of California, there are only 17 beds per 100,000 residents.
In January, the supervisors approved a motion that directed LA County Department of Mental Health Director Jonathan Sherin to return with a comprehensive report on how best to address the county’s shortage of mental health hospital beds.
Dr. Sherin’s report notes that shortage of mental health emergency services leaves patients in overcrowded waiting rooms in psychiatric emergency rooms, stuck — sometimes for days — while they wait for hospital beds to become available.
And once people make it into the hospital, they often become stuck there, too, because there aren’t enough community beds and services into which they can be transferred when they no longer need hospital care, but still need treatment.
Additionally, between four and five thousand people with serious mental illness are locked inside LA County’s jail system. “Many of their incarcerations could have been prevented entirely had they received needed treatment,” the report states.
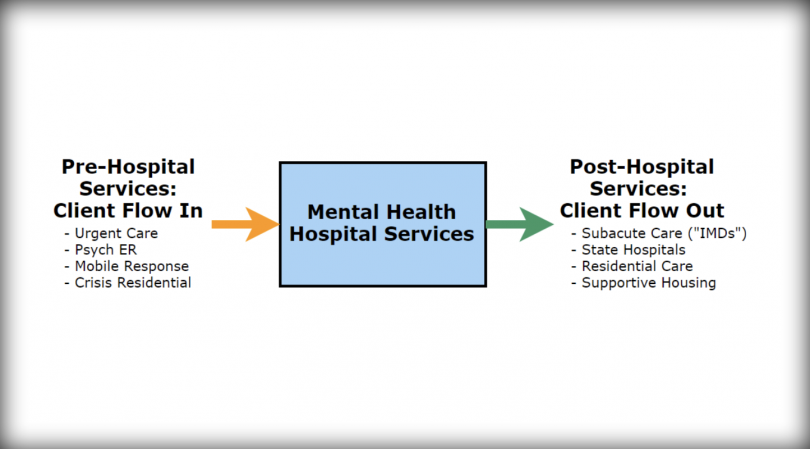
Working with the CEO’s office and other relevant departments and experts, Dr. Sherin found that increasing the number of hospital beds alone would not solve the county’s “dire” mental health crisis. Instead, to strengthen the “continuum of care,” county leaders must also boost access to “subacute” treatment and unlocked community residential treatment services for patients that need assistance beyond a short-term hospital stay. The county must also expand the services available to “treat clients in crisis and provide alternatives to hospitalization and/or incarceration.”
In his report, Sherin also stressed the importance of improving the quality of care that patients receive, as well as the efficiency of the flow of clients through the available beds.
The DMH report called for a two-year pilot program through which the county will work to attain 500 mental health beds of varying types.
On Tuesday, the board of supervisors approved the plan.
This pilot program, said Supervisor Barger, “is a critical first step” to be followed by “rapid expansion” of public mental health care in the years to follow.
People in need of crucial psychiatric services in the northern reaches of LA County will also soon be served by a new High Desert Mental Health Urgent Care Center in Lancaster. The 9,000-square-foot facility, a first-of-its-kind in the county, would be open 24/7 to meet the needs of the community.
“This new state-of-the-art facility will provide our Antelope Valley residents with access to high-quality, low-cost mental health services including diagnosis, treatment, referrals, case management and crisis intervention,” Supervisor Kathryn Barger recently said.
The county’s push for expanded access to such treatment will hopefully help reduce homelessness among people with mental illness, as well as cut down on contact with law enforcement and jail time for people whose needs are best met through mental health treatment.

Total BS. Is this supposed to really impress someone. It’s like filling a crack in the San Andreas fault and expecting an “Ata boy”.
How many treatment beds would the Mental Health Treatment Center (MHTC) voted for and then against by the BOS have had? How much money was wasted on the research and planning of the replacement for the archaic, outdated and inhuman Men’s Central Jail that morphed into the MHTC? I guess the BOS takes full advantage of the short term memory plagued citizenry and their ignorance.
The boldness and downright contempt of politicians for the intelligence of the voters is at an all time high. A state of total disregard and disrespect is the new normal it would appear.