Prison employees experience Post Traumatic Stress Disorder at a rate that is similar to Iraq and Afghanistan war veterans and higher than police officers, according to a study by researchers at Washington State University and the University of Alabama-Birmingham that was recently published in the American Journal of Industrial Medicine.
The researchers sent surveys to each of the approximately 2,000 members of the union representing WA state prison workers. A total of 355 Washington State Department of Corrections staff, including guards, counselors, medical practitioners, and other staff, responded and participated in the study.
A total of 19 percent of the survey respondents met the criteria for a PTSD diagnosis—a rate that is six times higher than that of the general public, according to the report.
In comparison, approximately 11-20 percent of Iraq and Afghanistan war vets, and 30 percent of Vietnam veterans have experienced PTSD, according to the report.
“The violent and chaotic nature of prison work has been show to negatively impact prison employee physical health, mental health, sleep, personal life, and general wellness,” the researchers stated in their report. “[Prison employees] consistently face inconsistent and long work hours, challenging and confrontational workplace interactions, uncertain job responsibilities, violence, trauma, and threats to their personal safety. Yet despite these well-established problems, the prevalence, causes, and insulators of PTSD among prison employees have not been well studied.”
Although research on PTSD among correctional officers is still relatively rare, this study isn’t the first to look at the issue. A 2013 report from Desert Waters Correctional Outreach found that 31 percent of guards in correctional facilities suffer from PTSD. (The Desert Waters report looked specifically at guards, rather than all prison staff.)
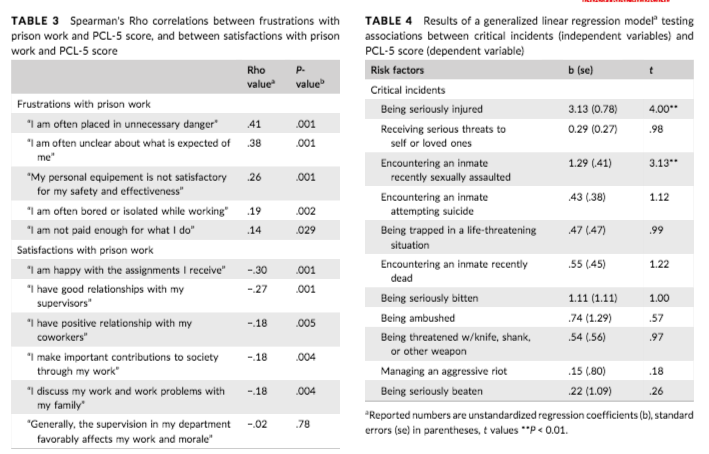
The recent Washington State/University of Alabama report found that factors like exposure to critical incidents corresponded with higher PTSD diagnosis checklist scores. Events like “being seriously injured,” and “encountering an inmate recently sexually assaulted” strongly correlated with higher PTSD scores. Other PTSD-connected incidents included “receiving serious threats to self or loved ones,” and “encountering an inmate attempting suicide.”
Workers who reported being “often placed in unnecessary danger,” and being “often unclear about what is expected” of them in the course of their jobs, also had higher PTSD scores.
The findings line up with a a 2016 study, which revealed that police officers’ exposure to critical incidents was “statistically significantly correlated” with drinking and PTSD. Those officers that had experienced a higher number of critical incidents were more likely to report having symptoms of PTSD and consuming alcohol.
As with war vets, shame and stigma often deter corrections officers and other law enforcement officers from seeking treatment for PTSD and other mental health needs.
For former Oregon Department of Corrections Sergeant Michael Van Patten, long-untreated PTSD—brought on by the trauma of witnessing and experiencing job-related violence—in combination and a macho correctional officer culture, led to a suicide attempt.
Van Patten and his son, who thwarted his father’s suicide attempt, have since recorded a video telling Michael’s story, and discussing the detrimental impacts of Michael’s internalized PTSD on his family. The Oregon DOC uses the video to educate staff about the importance of prioritizing their mental health care.
According to the California Correctional Peace Officers Association (CCPOA), the suicide rate for its members was 19.4 deaths per 100,000 in 2013.
In response to an alarming spate of suicides in their ranks, CCPOA together with researchers at the University of California, Berkeley, launched a study to assess the mental health needs of the state’s correctional officers. The study, which is still in progress, includes a survey completed by 8,600 corrections and parole officers statewide. Once their analysis is complete, CCPOA and Berkeley researchers plan to explore various pilot programs and mental health interventions.

I wonder if they separated out the responses from prison guards who ARE war vets because there are quite a few. That said, our prison culture in the US needs to change do that both staff and inmates are not traumatized and leave in more need of therapy.
If society could address the problem of people committing crimes we wouldn’t need a criminal justice system that has to rely on law enforcement and utilize jails/prisons. An ideal..not a reality though.
Prison workers, suffering from PTSD. Hmm…this was the reason why in the past, individuals who worked in the field had better pay and retirement benefits to make up for the physical risks. This was also an effort to attract people to the career and make up for the stress they incurred.
When the economy took a downturn, folks started getting laid off and having a hard time finding job, folks became critical of the “fat pensions” (as CF likes to say) and it started to become en vogue to blame all the ills of society on the the enforcement arm of the criminal justice system. A paradigm shift began.
Now no one wants these jobs, can’t pass the back ground exam and those already in it, are oftentimes being overworked due to staff shortages.
You don’t know what you are talking about. If you spent one hour as a correction officer, teacher, social worker or mental health facilitator, you would see what a difficult and stressful job it is and how you worry about if you will make it home to your family. Police and firefighters go through the same stress. You sound like some overeducated know it all that couldn’t take what these people endure. I was one of them for eight years. I have never recovered from what I experienced.
The risks and dangers associated with LE and Corrections is definitely there. Having worked both higher and lower level joints I can tell you the drama doesn’t end just changes. Higher level joints you’re always operating in the orange and red with inmate awareness, increasing internal stressors and higher levels of addiction and divorces for sure. The lower levels might operate more in the yellow zone but still “turned on”, but the stressors come more from Administration and being in the “fish bowl” due to a lack of other inmate issues going on, so Admin nit picks the crap out of the CO’s for petty shit that would never be an issue at the higher level joints.
I agree wholeheartedly on what you said. Having worked ASU for a decade and on the yards it doesn’t really matter where you’re at in the institution inmate b/s is inmate b/s. Inmate violence on each other, staff assaults, OIA investigations because of b/s inmate complaints and management’s constant nit-picking all add up to the “stressers”. This doesn’t even account for the “home” life and dealing with friends and family who don’t really understand or a society who does nothing but constantly put the inmate on a pedestal and have a false narrative that all C/O’s and staff are corrupt overpaid cry babies.
Just to think I was diagnosed with complex PTSD , basically PTSD on top of PTSD. First from the Military and then from a massive staff assault over at PBSP back in 2017! Double whammy!! No wonder Im lil messed up
me too only at folsom,wasnt very fun,long time ago but still see it like yesterday,it is real.
I agree to en extent. Research and data translates into numbers and the justification (data) that is needed to implement change in an archaic system. Data is also used to manipulate information so it is important to look at how the data was derived.
It is a shame how society is using the wages of hard working people as a way to correct fiscal mismanagement within a government system.
Resources are needed to increase access and decrease stigma of mental health services to those who need it.
Hi Sergio, I am medically retired from CMF; complex, cumulative PTSD. I would like to speak with you regarding PTSD.
Will CCPOA fight for retirees to receive extra pay for having PTSD similar
to veterans with this disorder?
Agreed. On top of this, Gavin Newsom deciding we don’t sacrifice enough so we need a 10 percent pay cut this year… meanwhile he continues to spout off about how much he supports healthcare workers, and with the hand behind his back he gives them a 10 percent pay cut (relevant because that means prison healthcare workers get salaries cut at the same time they pay higher and higher health insurance). Is that a sign of valuing them? Maybe he feels people will hear him on the news saying he supports healthcare workers, and the pay cut will be quietly brushed under the political table.
Was diagnose PTSD 3 years ago, just after early retirement (20 years). Working with counselors has helped a lot. My startle response and hyper-vigilance have improved significantly.
Found a great free application from the Veterans administration for anyone! It has several great tools to deal with many symptoms of PTSD. It is called “PTSD Coach”, and even has email follow-up features to remind you to check-in re: your current stress levels.
I use it and the application walks you through different meditation and multiple relaxation techniques. You can try different methods till you find one that works for you.
After Peacekeeper article on PTSD in last issue, I’m trying to get editors there to make CCPOA members aware, and contacting CCPOABTF to notify as many members as possible.
I’m on Facebook Messenger if you need more info.
I am going on 20 years with CDCR with experience in two level 4 prisons and one Reception. The experiences and incidents that I have seen in my almost 20 years is nothing I have ever seen prior to my employment with CDCR. I will admit this wasn’t the first choice career that I wanted to pursue, my original plan was to become a Cop on the streets however due to a knee injury I obtained during my military time prevented me becoming a Cop on the streets. It wasn’t until a relative who was an MTA at the time would always tell me different stories about work in a prison. Now here I am.
Those experiences and incidents which for the most part I will never forget and other things I will take to the grave with me. I have been involved in many incidents mainly Inmate on Inmate however there have been a few Inmate on Staff incidents that I either was part of or responded to.
There has been numerous times early on in my career that I found myself looking at other jobs wishing that if I didn’t have this knee injury I would of been a Cop on the streets. So yes for the past almost 20 years, I do suffer Depression at times. I may even have PTSD from this job. The experiences and incidents working in a prison are things you will never see in a normal life with a normal job.
The things that I once enjoyed when I was in the Army like going out with the guys to the clubs is something I won’t do anymore. I can’t stand tight spaces such as being on a dance floor when you are bumping into other people not knowing if accidently bumping into someone will set them off and end up in a altercation. So now I keep my circle small which is mainly family.
Now with this pandemic and now the federal ruling that all CDCR staff will be mandated to be vaccinated against Covid-19 isn’t something I am willing to do. Now I am finding myself again looking at jobs out of California. Instead of a regular retirement now I might have to pursue other options due to CDCR using (Duress, Bullying, Threating) of Adverse Action for those employees who refuse to be vaccinated. All the government cares about is the numbers of vaccinations yet they don’t realize that even vaccinated people are still getting the Covid-19 and in some cases people are experiencing heart problems after getting the vaccine. This is why people who are not vaccinated are choosing not to be vaccinated like me.
I look at one of the last pandemics (The Flu) which was one of the most deadly of human life and until this day people still die from the Flu. Now the Flu vaccine isn’t mandatory for CDCR staff however a vaccine for Covid-19 that has not been approved except for Emergency Use Only by the FDA is being mandated and in some jobs now a condition of employment. Unfortunately to say that this Covid-19 isn’t going anywhere and is going to continue to take lives for many years to come just like the Flu.
The Government needs to stop with all these mandates and let people choose for themselves…this doesn’t help when people who suffer from Mental Disorders and who choose not to be vaccinated. What happened to the right to refuse medical treatment?? Inmates all day long can refuse any medical treatment however any CDCR staff cannot in regards to Covid-19.
I am a surviving spouse of Correctional officer suicide. His job had forced overtime 16 hour shifts back to back because no one wanted to live In Susanville where there were 2 prisons. The town was small and rural and there is not adequate support or services for these guards and the town being so small seemed to know everyone and their personal life so this was a problem with anyone to try to get help for fear and the stigma of being a weak or problem employee. The overtime was not worth it when the State takes half of it in taxes. I tried to just get a tour of the inside of the prisons to understand what my husband was going through and was never given the opportunity. He would wake up swinging and was becoming more and more angry, tired and frusterated with me and our 3 daughters. It was so uncomfortable when he was home that after getting counseling I decided to seperate from him. It came down to he needed to quit his job or something had to change. I worked full-time at child support which probably scared him and added more stress because he was afraid of what I might do to him like he has heard from other co-workers. I honestly wouldn’t ever put anyone into the child support court and believe after a caseload of 750 that Child Support and CPS are just tools to make a family problem worse. It is a way to hurt and punish each other instead of finding solutions that unite not fight each other. Programs like successful uncoupling and trying to co-parent with forgiveness and acceptance are better options. How do you even do any type of counseling when you work 24-7. It’s inhumane. I wish I could go back and change what I lost. He was a totally different person when we met. My daughters and I were attacked by Sheriff and CPS when we moved to my hometown an hour away and our daughters I had to adopt out or having them suffer more traumatic crap from law enforcement and social workers who had no idea what we had really just walked through. No support and No protection from people seeking to get something from a vulnerable family for their own benefit whether it be public or employment advancement or financial. While causing a rift and misunderstanding between me and my three daughters who should have been left to grieve and grow in peace.
PTSD is Definitely an Issue With Correctional Officers Who Are Not Protected By The Administration When They See Wrongdoings Amongst The Work Environment. They Then Become Whistleblower’s and Are Labeled a “Rat/Snitch,” and are Left All Alone to Defend Themselves by The Rogue Officer’s Trying To Do Harm to Them. The Green Wall is a Major Issue Within The Walls of the CDCR.
It is funny how they can talk about this and still screw us at work. Our contacts get worse and the union gets lazzy. The help we may get is not there. They say they try and that is all they do is try. Put a camera on a monkey and take money from them for doing their job. It is sad how bad this job has been getting over the years. Everyday they lie, every day it gets worse